Myalgic encephalomyelitis/chronic fatigue syndrome
Myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is a serious long-term illness. People with ME/CFS experience a profound fatigue that does not go away with rest, sleep issues and problems with memory or concentration. They are able to do much less than before they became ill. Further common symptoms include dizziness, nausea and pain.[3] The hallmark symptom is a worsening of the illness hours to days after minor physical or mental activity. This "crash" can last less than a day to several months.[10]
| Myalgic encephalomyelitis/chronic fatigue syndrome | |
|---|---|
| Other names | Post-viral fatigue syndrome (PVFS), systemic exertion intolerance disease (SEID)[1]: 20 |
| The four primary symptoms of ME/CFS according to the National Institute for Health and Care Excellence | |
| Specialty | Rheumatology, rehabilitation medicine, endocrinology, infectious disease, neurology, immunology, general practice, paediatrics, other specialists in ME/CFS[2]: 58 |
| Symptoms | Worsening of symptoms with activity, long-term fatigue, sleep problems, others[3] |
| Usual onset | Peaks at 10–19 and 30–39 years old[4] |
| Duration | Long-term[5] |
| Causes | Unknown[6] |
| Risk factors | Being female, family history, viral infections[6] |
| Diagnostic method | Based on symptoms[7] |
| Treatment | Symptomatic[8] |
| Prevalence | About 0.17% to 0.89% (pre-pandemic)[9] |
The cause or causes of the disease are unknown.[11] ME/CFS often starts after an infection, such as mononucleosis.[12] ME/CFS can run in families, but no genes that contribute to ME/CFS have been found.[13] ME/CFS is associated with changes in the nervous and immune systems, as well as in energy production.[14] Diagnosis is based on symptoms because no diagnostic test is available.[7]
The illness can improve or worsen over time, but full recovery is uncommon.[12] Treatment is aimed at relieving symptoms, as no therapies or medications are approved to treat the condition.[2]: 29 Pacing one's activities can help avoid flare-ups and counselling may help in coping with the illness.[8] Before the COVID-19 pandemic, ME/CFS affected roughly one in every 150 people, although estimates varied widely.[9] However, many people with long COVID fit ME/CFS diagnostic criteria.[15] ME/CFS occurs more often in women than in men. It most commonly affects adults between ages 40 and 60 but can occur at other ages, including childhood.[16]
ME/CFS has a large social and economic impact. About a quarter of individuals are severely affected and unable to leave their bed or home.[10]: 3 The disease can be socially isolating.[17] People with ME/CFS often face stigma in healthcare settings and care is complicated by controversies around the cause and treatments of the illness.[18] Doctors may be unfamiliar with ME/CFS, as it is often not fully covered in medical school.[15] Historical research funding for ME/CFS has been far below that of diseases with comparable impact.[19]
Classification
ME/CFS has been classified as a neurological disease by the World Health Organization (WHO) since 1969, initially under the name benign myalgic encephalomyelitis.[20] In the WHO's most recent classification, the ICD-11, both chronic fatigue syndrome and myalgic encephalomyelitis are named under post-viral fatigue syndrome, classified under other disorders of the nervous system.[21]
The cause of the illness is unknown and the classification is based on symptoms which indicate a central role of the nervous system.[22] Alternatively, based on abnormalities in immune cells, ME/CFS may better fit into a classification of a neuroimmune condition.[23]
Some people with post-acute infection syndrome (PAIS) meet the criteria of ME/CFS. PAISs such as long COVID and post-treatment Lyme disease syndrome share many symptoms with ME/CFS and are suspected to have a similar cause. The term post-infectious fatigue syndrome describes severe fatigue after an infection, often with additional signs and symptoms. It was initially considered a subset of chronic fatigue syndrome with a documented triggering infection. There is no agreement on which conditions the term should encompass.[24]
Signs and symptoms
The illness causes debilitating fatigue, sleep problems, and post-exertional malaise (PEM, overall symptoms getting worse after mild activity). In addition, cognitive issues, orthostatic intolerance (dizziness or nausea when upright), or other symptoms, may be present (see also § Diagnostic criteria). Symptoms significantly reduce the ability to function compared to before the illness started and typically last for three to six months before a diagnosis can be confirmed.[10]: 13 [2]: 11 The onset of ME/CFS may be gradual or sudden.[1] When it begins suddenly, it often follows an infection.[1]: 158
Debilitating fatigue
People with ME/CFS experience persistent debilitating fatigue. It is made worse by normal physical, mental, emotional, and social activity, and is not a result of ongoing overexertion.[3][2]: 12 Rest provides limited relief from fatigue. Particularly in the initial period of illness, this fatigue is described as "flu-like". Individuals may feel restless and describe their experience as "wired but tired". When starting an activity, muscle strength may drop rapidly, which can lead to difficulty with coordination, clumsiness or sudden weakness.[2]: 12, 57 Mental fatigue may make cognitive efforts difficult. The fatigue experienced in ME/CFS is of a longer duration and greater severity than in other conditions characterized by fatigue.[10]: 5–6
Post-exertional malaise
The hallmark feature of ME/CFS is a worsening of symptoms after exertion, known as post-exertional malaise. PEM involves increased fatigue and is disabling. It can also include flu-like symptoms, pain, cognitive difficulties, gastrointestinal issues, nausea, and sleep problems.[10]: 6 The term malaise may be considered outdated, as it can give the impression of just a "vague discomfort"; the term post-exertional symptom exacarbation may capture the symptom better.[25]: 49
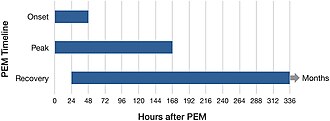
All types of activities that require energy, whether physical, cognitive, social, or emotional, can trigger PEM.[25]: 49 Examples include attending a school event, a grocery run, or even taking a shower.[3] For some, being in a stimulating environment can be sufficient to trigger PEM.[25]: 49 PEM usually starts 12 to 48 hours after the activity,[26] but can also follow immediately after. PEM can last hours, days, weeks, or months.[10]: 6 Extended periods of PEM, commonly referred to as "crashes" or "flare-ups," can lead on to a prolonged relapse.[25]: 50
Sleep problems
Unrefreshing sleep is a further core symptom. People wake up exhausted and stiff rather than restored after a night's sleep. This can be caused by a pattern of sleeping during the day and being awake at night, shallow sleep, or broken sleep. However, even a full night's sleep is typically non-restorative. Some individuals experience insomnia, hypersomnia (excessive sleepiness), or vivid nightmares.[25]: 50
Cognitive dysfunction
Cognitive dysfunction in ME/CFS can be as disabling as physical symptoms, leading to difficulties at work or at school, as well as in social interactions.[10]: 7 People with ME/CFS sometimes describe it as "brain fog",[3] and report a slowdown in information processing.[10]: 7 Individuals may have difficulty speaking, struggling to find words and names. They may have trouble concentrating or multitasking, or may have difficulties with short-term memory.[2] Tests often show problems with short-term visual memory, reaction time and reading speed. There may also be problems with attention and verbal memory.[27]
Orthostatic intolerance
People with ME/CFS often experience orthostatic intolerance, symptoms that start or worsen with standing or sitting. Symptoms, which include nausea, lightheadedness, and cognitive impairment, often improve again after lying down.[12] Weakness and vision changes may also be triggered by the upright posture.[3] Some have postural orthostatic tachycardia syndrome (POTS), an excessive increase in heart rate after standing up, which can result in fainting.[10]: 7 Additionally, individuals may experience orthostatic hypotension, a drop in blood pressure after standing.[28]: 17
Other common symptoms
Pain and hyperalgesia (an abnormally increased sensitivity to pain) are common in ME/CFS. The pain is not accompanied by swelling or redness.[28]: 16 The pain can be present in muscles (as myalgia) and joints. Individuals with ME/CFS may have chronic pain behind the eyes and in the neck, as well as neuropathic pain (related to disorders of the nervous system).[10]: 8 Headaches and migraines that were not present before the illness can occur as well. However, chronic daily headaches may indicate an alternative diagnosis.[28]: 16
Additional common symptoms include irritable bowel syndrome or other problems with digestion, chills and night sweats, shortness of breath or an irregular heartbeat. Some experience sore lymph nodes and a sore throat. People may also develop allergies or become sensitive to foods, lights, noise, smells or chemicals.[3]
Severity
ME/CFS often leads to serious disability, but the degree varies considerably.[11] ME/CFS is generally classified into four categories of illness severity:[2]: 8 [28]: 10
- People with mild ME/CFS can usually still work and care for themselves, but they will need their free time to recover from these activities rather than engage in social and leisure activities.
- Moderate severity impedes activities of daily living (self-care activities, such as making a meal). People are usually unable to work and require frequent rest.
- People with severe ME/CFS are homebound and can do only limited activities of daily living, for instance brushing their teeth. They may be wheelchair-dependent and spend the majority of their time in bed.
- With very severe ME/CFS, people are mostly bedbound and cannot care for themselves.
Roughly a quarter of those living with ME/CFS fall into the mild category, and half fall into the moderate or moderate-to-severe categories.[6] The final quarter falls into the severe or very severe category.[10]: 3 Severity may change over time. Symptoms might get worse, improve or the illness may go into remission for a period.[11] People who feel better for a period may overextend their activities, triggering PEM and a worsening of symptoms.[26]
Those with severe and very severe ME/CFS experience more extreme and diverse symptoms. They may face severe weakness and be unable to move at times.[29] They can lose the ability to speak, swallow, or communicate completely due to cognitive issues. They can further experience severe pain and hypersensitivities to touch, light, sound, and smells.[2]: 50 Exposure can lead to an increase in symptoms, in particular pain. The activities that can trigger PEM in the severely ill are very minor, such as sitting or going to the toilet.[29]
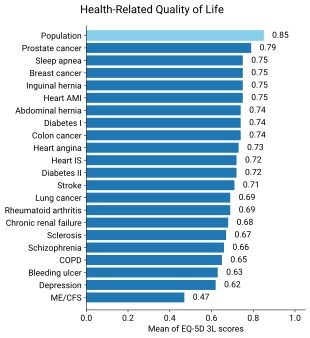
People with ME/CFS have decreased quality of life according to the SF-36 questionnaire, especially in the domains of physical and social functioning, general health, and vitality. However, their emotional functioning and mental health are not much lower than healthy controls.[30] Functional impairment can be greater than multiple sclerosis, heart disease, or lung cancer.[12] Fewer than 50% of people with ME/CFS are employed, and 19% have a full-time job.[9]
Causes
The cause of ME/CFS is not yet known.[12] Between 60% and 80% of cases start after an infection, usually a viral infection.[28]: 5 [6] A genetic factor is believed to contribute, but there is not a single gene responsible for increased risk.[13] Problems with the nervous and immune systems and energy metabolism may be factors.[12] ME/CFS is a biological disease, not a psychological condition,[30][11] and is not due to deconditioning.[30][12]
Besides viruses, other reported triggers include stress, traumatic events, and environmental exposures such as mould.[10]: 21 Bacterial infections such as Q-fever are other potential triggers.[28]: 5 ME/CFS may further occur after physical trauma, such as an accident or surgery.[11] Pregnancy has been reported in around 3% to 10% of cases as a trigger.[31] ME/CFS can also begin with multiple minor triggering events, followed by a final trigger that leads to a clear onset of symptoms.[6]
Risk factors
ME/CFS can affect people of all ages, ethnicities, and income levels, but it is more common in women than men.[9] People with a history of frequent infections are more likely to develop it.[14] Those with family members who have ME/CFS are also at higher risk, suggesting a genetic factor.[13] In the United States, white Americans are diagnosed more frequently than other groups,[32] but the illness is probably at least as prevalent among African Americans and Hispanics.[16] It used to be thought that ME/CFS was more common among those with higher incomes. Instead, people in minority groups or lower income groups may have increased risks due to poorer nutrition, lower healthcare access, and increased work stress.[9]
Viral infections
Viral infections have long been suspected to cause ME/CFS, based on the observation that ME/CFS sometimes occurs in outbreaks and is possibly connected to autoimmune diseases.[33] How viral infections cause ME/CFS is unclear; it could be via viral persistence or via a "hit and run" mechanism, in which infections dysregulate the immune system or cause autoimmunity.[34]
Different types of viral infection have been implicated in ME/CFS, including airway infections, bronchitis, gastroenteritis, or an acute "flu-like illness".[10]: 226 Between 15% and 50% of people with long COVID also meet the diagnostic criteria for ME/CFS.[10]: 228 Of people who get infectious mononucleosis, which is caused by the Epstein–Barr virus (EBV), around 8% to 15% develop ME/CFS, depending on criteria.[10]: 226 Other viral infections that can trigger ME/CFS are the H1N1 influenza virus, varicella zoster (the virus that causes chickenpox and shingles), and SARS-CoV-1.[35]
Reactivation of latent viruses, in particular EBV and human herpesvirus 6, has also been hypothesised to drive symptoms. EBV is present in about 90% of people, usually in a latent state.[36][37]: 13 The levels of antibodies to EBV are commonly higher in people with ME/CFS, indicating possible viral reactivation.[38]
Pathophysiology
ME/CFS is associated with changes in several areas, including the nervous and immune systems, as well as disturbances in energy metabolism.[11][14] Neurological differences include autonomic nervous system dysfunction and a change in brain structure and metabolism.[39] Observed changes in the immune system include decreased natural killer cell function and, in some cases, autoimmunity.[14]
Neurological
A range of structural, biochemical, and functional abnormalities are found in brain imaging studies of people with ME/CFS.[23][39] Common findings are changes in the brainstem and the use of additional brain areas for cognitive tasks. Other consistent findings, based on a smaller number of studies, are low metabolism in some areas, reduced serotonin transporters, and problems with neurovascular coupling.[22]
Neuroinflammation has been proposed as an underlying mechanism of ME/CFS that could explain a large set of symptoms. A number of studies suggest neuroinflammation in the cortical and limbic regions of the brain. People with ME/CFS, for instance, have higher brain lactate and choline levels, which are signs of neuroinflammation. More direct evidence from two small PET studies of microglia, a type of immune cell in the brain, were contradictory, however.[40][41]
ME/CFS affects sleep. People with ME/CFS experience decreased sleep efficiency, take longer to fall asleep, and take longer to achieve REM sleep, a phase of sleep characterised by rapid eye movement. Changes to non-REM sleep have also been found, together suggesting a role of the autonomic nervous system.[42] Individuals often have an blunted heart rate response to exercise, but a higher heart rate during a tilt table test when the body is rotated from lying flat to an upright position. This again suggests dysfunction in the autonomic nervous system.[43]
Immunological
People with ME/CFS often have immune system abnormalities. A consistent finding in studies is a decreased function of natural killer cells, a type of immune cell that targets virus-infected and tumour cells.[44] T cells show less metabolic activity. This may reflect they have reached an exhausted state and cannot respond effectively against pathogens.[14] People with ME/CFS have an abnormal response to exercise. This includes increased production of complement products, increased oxidative stress combined with a decreased antioxidant response, and increased interleukin 10 and TLR4. Some of these changes correlate with symptom severity.[45]
Autoimmunity has been proposed to be a factor in ME/CFS. There is a subset of people with ME/CFS with increased levels of autoantibodies, possibly as a result of viral mimicry.[46] Some may have higher levels of autoantibodies to muscarinic acetylcholine receptors as well as to β2 adrenergic receptors.[46][14] Problems with these receptors can lead to impaired blood flow.[47]
Energy

Objective signs of PEM have been found with the 2-day cardiopulmonary exercise test.[48] People with ME/CFS have lower performance compared to healthy controls on the first test. On the second test, healthy people's scores stay the roughly the same or increase slightly, while those with ME/CFS have a clinically significant decrease in work rate at the anaerobic threshold. Potential causes include mitochondrial dysfunction, and issues with transport and use of oxygen.[49]
Studies have observed mitochondrial abnormalities in cellular energy production, but differences between studies make it hard to draw clear conclusions.[50] ATP, the primary energy carrier in cells, is likely more frequently produced from lipids and amino acids than from carbohydrates.[14]
Other
Some people with ME/CFS have abnormalities in their hypothalamic–pituitary–adrenal axis hormones. This can include lower cortisol levels, less change in cortisol levels throughout the day, and a weaker reaction to stress and stimuli.[51] Other proposed abnormalities are reduced blood flow to the brain under orthostatic stress (as found in a tilt table test), small-fibre neuropathy, and an increase in the amount of gut microbes entering the blood.[28]: 9 The diversity of gut microbes is reduced compared to healthy controls.[14] Women with ME/CFS are more likely to experience endometriosis, early menopause, and other menstrual irregularities compared to women without the condition.[11]
Diagnosis
Diagnosis of ME/CFS is based on symptoms[7] and involves taking a medical history and a mental and physical examination.[52] No specific lab tests are approved for diagnosis; while physical abnormalities can be found, no single finding is considered sufficient for diagnosis.[12][7] Blood and urine tests are used to rule out other conditions that could be responsible for the symptoms.[52] People with ME/CFS often face significant delays in obtaining a diagnosis and diagnoses may be missed altogether.[2]: 66 Specialists in ME/CFS may be asked to confirm the diagnosis, as primary care physicians often lack a good understanding of the illness.[2]: 68
Diagnostic criteria
| Symptom M: Mandatory O: Optional | Fukuda | CCC | ICC | IOM | NICE |
|---|---|---|---|---|---|
| Fatigue | M | M | M | M | M |
| Functional impairment | M | M | M | M | M |
| PEM | O | M | M | M | M |
| Sleep problems | O | M | O | M | M |
| Cognitive issues | O | O | O | O | M |
| Pain or headaches | O | M | O | ||
| Orthostatic intolerance | O | O | O | ||
| Flu or cold symptoms | O | O | O | ||
| Nausea | O | O | |||
| Cardiovascular problems | O | O | |||
| Hypersensitivities | O | O | |||
| Susceptibility to infection | O |
Multiple research and clinical criteria exist to diagnose ME/CFS. These include the NICE guidelines, IOM criteria, the International Consensus Criteria (ICC), the Canadian Consensus Criteria (CCC), and CDC criteria. The criteria sets were all developed based on expert consensus and differ in the required symptoms and which conditions preclude a diagnosis of ME/CFS.[28]: 14 The definitions differ in their conceptualisation of the cause and mechanisms of ME/CFS.[53]
As there is no biomarker for ME/CFS, it is not possible to determine which set of criteria are the most accurate. A trade-off must be made between missing more diagnoses and overdiagnosis. The broad Fukuda criteria have a higher risk over overdiagnosis, whereas the strict ICC criteria have a higher risk of missing people. The IOM and NICE criteria fall in the middle.[25]: 47–48
The 1994 CDC criteria, sometimes called the Fukuda criteria, require six months of persistent or relapsing fatigue for diagnosis, as well as the persistent presence of four out of eight other symptoms.[28]: 35 While used frequently, the Fukuda criteria have limitations: PEM and cognitive issues are not mandatory. The large variety of optional symptoms can lead to diagnosis of individuals who differ significantly from each other.[10]: 15
The Canadian Consensus Criteria, another commonly used criteria set, was developed in 2003.[28]: 14 In addition to PEM and sleep problems, pain and neurological or cognitive issues are required for diagnosis. Furthermore, three categories of symptoms are defined (orthostatic, thermal instability, and immunological). At least one symptom in two of these categories needs to be present.[10]: 15 [28]: 34 People diagnosed under the CCC have more severe symptoms compared to those diagnosed under the 1994 CDC criteria. Similarly, the International Consensus Criteria are stricter than the Fukuda criteria and select more severely ill people.[28]: 14
The 2015 criteria by the Institute of Medicine share significant similarities with the CCC but were developed to be easy to use for clinicians. Diagnosis requires fatigue, PEM, non-restorative sleep, and either cognitive issues (such as memory impairment) or orthostatic intolerance. Additionally, fatigue must persist for at least six months, substantially impair activities in all areas of life, and have a clearly defined onset.[10]: 16–17 Symptoms must be present at least half of the time, and be of moderate severity or worse; previous criteria just required symptoms to be present.[28]: 14 In 2021, NICE revised its criteria based on the IOM criteria. The updated criteria require fatigue, PEM, non-restorative sleep, and cognitive difficulties persisting for at least three months.[10]: 16–17
Separate diagnostic criteria have been developed for children and young people. A diagnosis for children often requires a shorter symptom duration. For example, the CCC definition only requires three months of persistent symptoms in children compared to six months for adults.[10]: 17–18 NICE requires only four weeks of symptoms to suspect ME/CFS in children, compared to six weeks in adults.[28]: 15 Exclusionary diagnoses also differ; for instance, children and teenagers may have anxiety related to school attendance, which could explain symptoms.[10]: 17–18
Clinical assessment

Screening can be done using the DePaul Symptom Questionnaire, which assesses the frequency and severity of ME/CFS symptoms.[28]: 24 Individuals may struggle to answer questions related to PEM, if they are unfamiliar with the symptom. To find patterns in symptoms, they may be asked to keep a diary.[12]
A physical exam may appear completely normal, particularly if the individual has rested substantially before a doctor’s visit.[12] There may be tenderness in the lymph nodes and abdomen or signs of hypermobility.[28]: 17 Answers to questions may show a temporary difficulty with finding words or other cognitive problems.[6] Cognitive tests and a two-day cardiopulmonary exercise test (CPET) can be helpful to document aspects of the illness, but they may be risky as they can cause severe PEM. They may be warranted to support a disability claim.[12] However, a two-day CPET cannot be used to rule out ME/CFS.[1]: 216 Orthostatic intolerance can be measured with a tilt table test. If that is unavailable, it can also be assessed with the simpler NASA 10-minute lean test, which tests the response to prolonged standing.[6]
Standard laboratory findings are usually normal. Standard tests when suspecting ME/CFS include a full blood count, a HIV test, red blood cell sedimentation rate (ESR), C-reactive protein, blood glucose and thyroid-stimulating hormone. Tests for antinuclear antibodies may come back positive, but below the levels that suggest the individual may have lupus. C-reactive protein levels are often at the high end of normal. Serum ferritin levels may be useful to test, as borderline anaemia can make some ME/CFS symptoms worse.[28]: 18
Differential diagnosis
Some medical conditions have symptoms similar to ME/CFS. Diagnosis often involves clinical evaluation, testing, and specialist referrals to identify the correct condition. During the time other possible diagnoses are explored, advice can be given on symptom management to help prevent the condition from getting worse.[2]: 66–67 A waiting period before ME/CFS is confirmed, is used to exclude acute medical conditions or symptoms which may resolve within that time frame.[12]
Possible differential diagnoses span a large set of specialties and depend on the medical history.[12] Examples are infectious diseases, such as Epstein–Barr virus and Lyme disease, and neuroendocrine disorders, including diabetes and hypothyroidism. Blood disorders, such as anaemia, and some cancers may also present similar symptoms.[12][25]: 57
Various rheumatological and autoimmune diseases, such as Sjögren's syndrome, lupus, and arthritis, may have overlapping symptoms with ME/CFS. Furthermore, it may be necessary to evaluate psychiatric diseases, such as depression or substance use disorder, as well as neurological disorders, such as narcolepsy, multiple sclerosis, and craniocervical instability.[12][25]: 57 Finally, sleep disorders, coeliac disease, and side effects of medications may also explain symptoms.[12]
Joint and muscle pain without swelling or inflammation is a common feature of ME/CFS, but is more closely associated with fibromyalgia. Modern definitions of fibromyalgia not only include widespread pain but also fatigue, sleep disturbances, and cognitive issues. This makes it difficult to distinguish ME/CFS from fibromyalgia[54]: 13, 26 and the two are often co-diagnosed.[28]: 28
Another common condition that often co-occurs with ME/CFS is hypermobile Ehlers–Danlos syndrome (EDS).[25]: 57 Unlike ME/CFS, EDS is present from birth. People with ME/CFS are more often hypermobile compared to the general population.[28]: 28–29 Sleep apnoea is may also co-occur with ME/CFS.[28]: 16 However, many diagnostic criteria require ruling out sleep disorders before confirming a diagnosis of ME/CFS.[10]: 7
Like with other chronic illnesses, depression and anxiety co-occur frequently with ME/CFS. Depression may be differentially diagnosed by the presence of feelings of worthlessness, the inability to feel pleasure, loss of interest, and/or guilt, and the absence of ME/CFS bodily symptoms such as autonomic dysfunction, pain, migraines, and PEM.[28]: 27 People with chronic fatigue, which is not due to ME/CFS or other chronic illnesses, may be diagnosed with idiopathic (unexplained) chronic fatigue.[28]: 32
Management
There is no approved drug treatment or cure for ME/CFS, although some symptoms can be treated or managed. Care for ME/CFS is multidisciplinary. Usually, the primary care clinician plays an important role in coordinating health care, social care and educational support for those still in school. This coordinator can help provide access to community resources such as occupational therapy and district nursing. Management may start with treating the most disabling symptom first, and tackle symptoms one by one in further health care visits.[28]: 46
Pacing, or managing one's activities to stay within energy limits, can reduce episodes of PEM. Addressing sleep problems with good sleep hygiene, or medication if required, may be beneficial. Chronic pain is common in ME/CFS, and the CDC recommends consulting with a pain management specialist if over-the-counter painkillers are insufficient. For cognitive impairment, adaptations like organisers and calendars may be helpful.[8]
Co-occurring conditions that may interact with and worsen ME/CFS symptoms are common, and treating these may help manage ME/CFS. Commonly diagnosed ones include fibromyalgia, irritable bowel syndrome, allergies, and chemical sensitivities.[55] The debilitating nature of ME/CFS can cause depression, anxiety, or other psychological problems, which can be treated.[8] People with ME/CFS may be unusually sensitive to medications, especially ones that affect the central nervous system.[56]
Pacing and energy management

Pacing, or activity management, involves balancing periods of rest with periods of activity.[26] The goal of pacing is to stabilize the illness and avoid triggering PEM.[57] This involves staying within an individual's available energy envelope to reduce the PEM "payback" caused by overexertion.[58] It was developed for ME/CFS in the 1980s.[59]
Pacing can involve breaking up large tasks into smaller ones and taking extra breaks, or creating easier ways to do activities. For example, avoiding standing by using a shower chair. The decision to stop an activity (and rest or change an activity) is determined by self-awareness of a worsening of symptoms. Use of a heart rate monitor may help some individuals with pacing.[8]
Research on pacing and energy envelope theory typically shows positive effects.[58][60] However, these studies have often been small and have rarely included methods to check if study participants implemented pacing well.[60] Pacing is difficult to apply for people with very severe ME/CFS, as the activities that trigger PEM in this group, such as eating, cannot be avoided completely.[57]
Those with a stable illness who understand how to "listen to their body" may be able to carefully and flexibly increase their activity levels.[26] The goal of the exercise programme would be to increase stamina, while not interfering with everyday tasks or making the illness more severe.[28]: 56 In many chronic illnesses, intense exercise is beneficial, but in ME/CFS it is not recommended. The CDC states:[8]
Vigorous aerobic exercise can benefit people with many chronic illnesses. But people with ME/CFS do not tolerate such exercise routines. Standard exercise recommendations for healthy people can be harmful for patients with ME/CFS. However, it is important that patients with ME/CFS undertake activities that they can tolerate.
Graded exercise therapy (GET), a proposed treatment for ME/CFS that assumes deconditioning and a fear of activity play important roles in maintaining the illness, is no longer recommended for people with ME/CFS.[6][28]: 38 Reviews of GET either see weak evidence of a small to moderate effect[61][62] or no evidence of effectiveness.[63][64] GET can have serious adverse effects.[57] Similarly, a form of CBT that assumed the illness is maintained by unhelpful beliefs about the illness and avoidance of activity, is no longer recommended.[12]
Symptom relief
The first management step for sleep problems in ME/CFS is improving sleep habits. If sleep problems remain after implementing sleep hygiene routines, cognitive behavioural therapy for insomnia can be offered. Avoiding naps during the day can further improve sleep,[28]: 41 but there may be a trade-off required rest during the day.[2]: 36 Drugs that help with insomnia in fibromyalgia, such as trazodone or suvorexant, may help in ME/CFS too.[6]
Pain is initially managed with over-the-counter pain medication, such as ibuprofen or paracetamol. If this is insufficient, referral to a pain specialist or counselling on pain management can be a next step. Heat treatment, hydrotherapy and gentle massage can sometimes help. In addition, stretching and exercise may help with pain, but a balance must be struck, as they can trigger PEM.[26] While there is lack of evidence on pharmaceutical options for pain management in ME/CFS, medication that works for fibromyalgia may be tried, such as pregabalin.[28]: 42 [6]
Like in other chronic illnesses, those with ME/CFS often experience mental health issues like anxiety and depression.[12] Psychotherapy, such as cognitive behavioural therapy (CBT) may help manage the stress of being ill and teach self-management strategies.[2]: 42 Family sessions may be useful to educate people close to those with ME/CFS about the severity of the illness.[28]: 41 Antidepressants can be useful, but there may be more side effects than in the general population. For instance, it may be difficult to stop weigth gain due to exercise intolerance.[28]: 52
Bowel issues are a common symptom of ME/CFS. For some, eliminating specific foods, such as caffeine, alcohol, gluten, or dairy, can alleviate symptoms.[12] A proper diet is a significant contributor to the health of any individual. Medical consultation about diet and supplements is recommended for people with ME/CFS.[65] Those with orthostatic intolerance can benefit from increased salt and fluid intake.[12] Compression stockings can help with orthostatic intolerance.[12]
Severe ME/CFS
People with moderate to severe ME/CFS may benefit from home adaptations and mobility aids, such as wheelchairs, disability parking, shower chairs, or stair lifts. To manage sensitivities to environmental stimuli, these stimuli can be limited. For instance, the surroundings can be made perfume-free, or an eye mask or earplugs can be used.[28]: 39–40 Those with severe ME/CFS may have significant trouble getting nutrition. Intravenous feeding (via blood) or tube feeding may be necessary to address this or to address electrolyte imbalances.[6]
Patients who cannot move easily in bed may need help to prevent pressure sores. Regular repositioning is important to keep their joints flexible, prevent stiffness and contractures. Osteoporosis may pose a risk over the long term.[66] Symptoms of severe ME/CFS may be misunderstood as neglect or abuse during well-being evaluations, and NICE recommends that professionals with experience in ME/CFS should be involved in any type of assessment for safeguarding.[2]: 22
Prognosis
Information on the prognosis of ME/CFS is limited. Complete recovery, partial improvement, and worsening are all possible,[11] but full recovery is uncommon.[10]: 11 Symptoms generally fluctuate over days, weeks, or longer periods, and some people may experience periods of remission. Overall, many will have to adjust to life with ME/CFS.[2]: 20
An early diagnosis may improve care and prognosis.[25] Factors that may make the disease worse over days, but also over longer time periods, are physical and mental exertion, a new infection, sleep deprivation, and emotional stress.[10]: 11 Some people who improve need to manage their activities in order to prevent relapse.[11] Children and teenagers are more likely to recover or improve than adults.[11][2]: 20 For instance, a study in Australia among 6- to 18-year-olds found that two-thirds reported recovery after ten years, and that the typical duration of illness was five years.[10]: 11
The effect of ME/CFS on life expectancy is poorly studied, and the evidence is mixed. One large retrospective study on the topic found no increase in all-cause mortality due to ME/CFS. Death from suicide was, however, significantly higher among those with ME/CFS.[28]: 59 In extreme cases, people can die from the illness.[57]
Epidemiology

Reported prevalence rates vary widely depending on how ME/CFS is defined and diagnosed. Overall, around 1 in 150 have ME/CFS. Based on the 1994 CDC diagnostic criteria, the global prevalence rate for CFS is 0.89%. In comparison, estimates using the stricter 1988 CDC criteria or the 2003 Canadian Consensus Criteria for ME produced a prevalence rate of only 0.17%.[9]
In England and Wales, over 250,000 people are estimated to be affected.[2]: 92 These estimates are based on data before the COVID-19 pandemic. It is likely that numbers have increased as a large share of people with long COVID meet the diagnostic criteria of ME/CFS.[10]: 228 A 2021–2022 CDC survey found that 1.3% of adults in the United States, or 3.3 million, had ME/CFS.[67]
Women are diagnosed about 1.5 to 4 times more often with ME/CFS than men.[9][16] The prevalence in children and adolescents is slightly lower than in adults,[9] and children have it less than adolescents.[68] The incidence rate has two peaks, one at 10–19 and another at 30–39 years,[4] and the prevalence is highest between ages 40 and 60.[30][16]
History
From 1934 onwards, there were multiple outbreaks globally of an unfamiliar illness, initially mistaken for polio. A 1950s outbreak at London's Royal Free Hospital led to the term "benign myalgic encephalomyelitis" (ME). Those affected displayed symptoms such as malaise, sore throat, pain, and signs of nervous system inflammation. While its infectious nature was suspected, the exact cause remained elusive.[1]: 28–29 The syndrome appeared in sporadic as well as epidemic cases.[69]
In 1970, two UK psychiatrists proposed that these ME outbreaks were psychosocial phenomena, suggesting mass hysteria or altered medical perception as potential causes. This theory, though challenged, sparked controversy and cast doubt on ME's legitimacy in the medical community.[1]: 28–29
Melvin Ramsay's later research highlighted ME's disabling nature, prompting the removal of "benign" from the name and the creation of diagnostic criteria in 1986. These criteria included the tendency of muscles to tire after minor effort and take multiple days to recover, high symptom variability, and chronicity. Despite Ramsay's work and a UK report affirming that ME was not a psychological condition, scepticism persisted within the medical field, leading to limited research.[1]: 28–29
In the United States, Nevada and New York State saw outbreaks of what appeared similar to mononucleosis in the middle of the 1980s. People suffered from "chronic or recurrent fatigue", among a large number of other symptoms.[1]: 28–29 The initial link between elevated antibodies and the Epstein–Barr virus led to the name "chronic Epstein–Barr virus syndrome". The CDC renamed it chronic fatigue syndrome (CFS), as a viral cause could not be confirmed in studies.[70]: 155–158 An initial case definition of CFS was outlined in 1988;[1]: 28–29 the CDC published new diagnostic criteria in 1994, which became widely referenced.[71]
In the 2010s, ME/CFS began to gain more recognition from health professionals and the public. Two reports proved key in this shift. In 2015, the Institute of Medicine produced a report with new diagnostic criteria that described ME/CFS as a "serious, chronic, complex systemic disease". Following this, the US National Institutes of Health published their Pathways to Prevention report, which gave recommendations on research priorities.[72]
Society and culture

Naming
Many names have been proposed for the illness. The most commonly used are "chronic fatigue syndrome", "myalgic encephalomyelitis", and the umbrella term "myalgic encephalomyelitis/chronic fatigue syndrome" (ME/CFS). Reaching consensus on a name is challenging because the cause and pathology remain unknown.[1]: 29–30
Many individuals with ME/CFS object to the term "chronic fatigue syndrome". They consider the term simplistic and trivialising, which in turn prevents the illness from being taken seriously.[1]: 234 [73] At the same time, there are also issues with the use of "myalgic encephalomyelitis" (myalgia means muscle pain and encephalomyelitis means brain and spinal cord inflammation), as there is only limited evidence of brain inflammation implied by the name.[28]: 3 The umbrella term ME/CFS would retain the better-known phrase CFS without trivialising the disease, but some people object to this name too, as they see CFS and ME as distinct illnesses.[73]
A 2015 report from the Institute of Medicine recommended the illness be renamed "systemic exertion intolerance disease" (SEID) and suggested new diagnostic criteria, proposing that PEM, impaired function, and sleep problems are core symptoms of ME/CFS.[1] While the new name was not widely adopted, the diagnostic criteria were taken over by the CDC. Like CFS, the name SEID only focuses on a single symptom, and opinion from those affected has generally been negative.[74]
Controversy
ME/CFS is a contested illness, with debates mainly revolving around the cause of the illness and treatments.[75] Historically, there was a heated discussion about whether the condition was psychological or neurological.[53] Professionals who subscribed to the psychological model had frequent conflicts with patients, who believed their illness to be organic.[18] While ME/CFS is now generally believed to be a multisystem neuroimmune condition,[53] a subset of professionals still see the condition as psychosomatic, or an "illness-without-disease".[18]
The possible role of chronic viral infection in ME/CFS has been a subject of disagreement. One study caused considerable controversy by establishing a causal relationship between ME/CFS and a retrovirus called XMRV. Some with the illness began taking antiretroviral drugs targeted specifically for HIV/AIDS, another retrovirus,[76] and national blood supplies were suspected to be tainted with the retrovirus. After several years of study, the XMRV findings were determined to be the result of contamination of the testing materials.[77]
Treatments based on behavioural and psychological models of the illness have also been the subject of much contention. The largest clinical trial on behavioural interventions, the 2011 PACE trial, concluded that graded exercise therapy and CBT are moderately effective. The trial drew heavy criticism.[75] The study authors weakened their definition of recovery during the trial: some participants now met a key criterion for recovery before the trial started. A reanalysis under the original clinical trial protocol showed no significant difference in recovery rate between treatment groups and the controls receiving standard care.[78][79]
Economic and social impact
ME/CFS negatively impacts people's social lives and relationships. Stress can be compounded by disbelief in the illness from the support network, who can be sceptical due to the subjective nature of diagnosis. Many people with the illness feel socially isolated, and thoughts of suicide are high, especially in those without a supportive care network.[17] ME/CFS interrupts normal development in children, making them more dependent on their family for assistance instead of gaining independence as they age.[80] Caring for somebody with ME/CFS can be a full-time role, and the stress of caregiving is made worse by the lack of effective treatments.[81]
Economic costs due to ME/CFS are significant.[82] In the United States, estimates range from $36 to $51 billion per year, considering both lost wages and healthcare costs.[83] A 2017 estimate for the annual economic burden in the United Kingdom was £3.3 billion.[13]
Advocacy

Patient organisations have aimed to involve researchers via activism but also by publishing research themselves—similarly to AIDS activism in the 1980s, which also sought to combat underfunding and stigma. Citizen scientists, for example, helped start discussions about weaknesses in trials of psychological treatments.[75]
ME/CFS International Awareness Day takes place on May 12.[84] The goal of the day is to raise awareness among the public and health care workers about the diagnosis and treatment of ME/CFS.[85] It was chosen because it is the birthday of Florence Nightingale, who had an unidentified illness similar to ME/CFS.[86]
Doctor–patient relations
The NAM report refers to ME/CFS as "stigmatized", and the majority of individuals report negative healthcare experiences.[1]: 30 They may feel that their doctor inappropriately calls their illness psychological or doubts the severity of their symptoms.[87] They may also feel forced to prove that they are legitimately ill.[88] Some may be given outdated treatments that provoke symptoms or assume their illness is due to unhelpful thoughts and deconditioning.[12]: 2871 [15]
Clinicians may be unfamiliar with ME/CFS, as it is often not fully covered in medical school.[15] Due to this unfamiliarity, people may go undiagnosed for years[12] or be misdiagnosed with mental health conditions.[15] As people with ME/CFS gain knowledge about their illness over time, their relationship with treating physicians changes. They may feel on a more equal footing with their doctors and able to work in partnership. At times, relationships may deteriorate instead as the previous asymmetry of knowledge breaks down.[17]
Research

Research into ME/CFS seeks to find a better understanding of the disease's causes, biomarkers to aid in diagnosis, and treatments to relieve symptoms.[1]: 10 The emergence of long COVID has sparked increased interest in ME/CFS, as the two conditions may share pathology and a treatment for one may treat the other.[23][14]
Research funding
Historical research funding for ME/CFS has been far below that of comparable diseases.[19][89] In a 2015 report, the US National Academy of Sciences said that "remarkably little research funding" had been dedicated to causes, mechanisms, and treatment.[1]: 9 Lower funding levels have led to a smaller number and size of studies.[90] In addition, drug companies have invested very little in the disease.[91]
The US National Institutes of Health (NIH) is the largest biomedical funder worldwide.[92] Using rough estimates of disease burden, a study found NIH funding for ME/CFS was only 3% to 7% of the average disease per healthy life year lost between 2015 and 2019.[93] Worldwide, multiple sclerosis, which affects fewer people and results in disability no worse than ME/CFS, received 20 times as much funding between 2007 and 2015.[89][19]
Multiple reasons have been proposed for the low funding levels. Diseases for which society "blames the victim" are frequently underfunded. This may explain why COPD, a severe lung disease often caused by smoking, receives low funding per healthy life year lost.[94] Similarly, for ME/CFS, the historical belief that it is caused by psychological factors may have contributed to lower funding. Gender bias may also play a role; the NIH spends less on diseases that predominantly affect women in relation to disease burden. Less well-funded research areas may also struggle to compete with more mature areas of medicine for the same grants.[93]
Research directions
Many biomarkers for ME/CFS have been proposed. Studies on biomarkers have often been too small to draw robust conclusions. Natural killer cells have been identified as an area of interest for biomarker research as they show consistent abnormalities.[7] Other proposed markers include electrical measurements of blood cells and Raman microscopy of immune cells.[14] Several small studies have investigated the genetics of ME/CFS, but none of their findings have been replicated.[13] A larger study, DecodeME, is currently underway in the United Kingdom.[95]
Various drug treatments for ME/CFS are being explored. Drugs under investigation often target the nervous system, the immune system, autoimmunity, or pain directly. More recently, there has been a growing interest in drugs targeting energy metabolism.[91] In several clinical trials of ME/CFS, rintatolimod showed a small reduction in symptoms, but improvements were not sustained after discontinuation.[96][91] Rintatolimod has been approved in Argentina.[97] Rituximab, a drug that depletes B cells, was studied and found to be ineffective.[14] Another option targeting autoimmunity is immune adsorption, which removes a large set of (auto)antibodies from the blood.[91]
Challenges
People with ME/CFS can widely differ in which symptoms they have and how severe these symptoms are. This poses a challenge for research into the cause and progression of the disease. Dividing people into subtypes may help manage this heterogeneity.[14] The existence of multiple diagnostic criteria and variations in how scientists apply them complicate comparisons between studies.[1]: 53 Definitions also vary in which co-occurring conditions preclude a diagnosis of ME/CFS.[1]: 52








